Frequently Asked Questions About Achilles Tendonitis
If you are a fan of professional sports and keep up with the related news, you occasionally hear of athletes or players having problems with their Achilles tendons. However, these issues do not just happen to professional athletes. They can impact you too, especially as you get older or if you participate in certain high-impact activities or sports. If you want to know more about Achilles tendonitis in particular, as well as learn how to diagnose, treat, and prevent it, keep reading to learn frequently asked questions as well as their answers.
What Is Achilles Tendonitis?
Before any conversation about this condition can get serious, it helps to know exactly what Achilles tendonitis is. In general, the definition of this affliction is an overuse injury of either Achilles tendon.
Where Is The Achilles Tendon Located?
The Achilles tendon is a band of tissue in the backs of your lower legs. These tendons connect your calf muscles to your lower heel bones. The easiest place to actually feel your Achilles tendon is on the back of your foot just above your heel and behind the ankle. If you cross one leg over a knee, put your thumb on the back of the crossed foot and start flexing your foot, pointing your toes up and down. Your thumb will feel the lower end of your Achilles tendon contracting and relaxing as you move your foot.
What Causes Achilles Tendonitis?
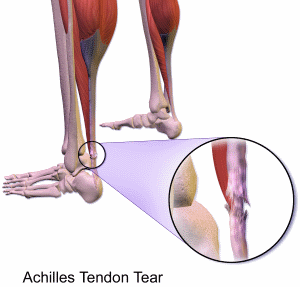 This injury most frequently plagues joggers and runners. In particular, it seems to hit those who recently went through a sudden increase in either the length or intensity of their running sessions.
This injury most frequently plagues joggers and runners. In particular, it seems to hit those who recently went through a sudden increase in either the length or intensity of their running sessions.
Middle-aged individuals known as ‘weekend warriors’ who only exercise on their days off are also at high risk of developing this injury. This is especially true of sports like basketball and tennis.
The reason that sports activities usually cause this injury is because of the function of the tendon. Since it is a physical connection between your heel bone and calf, you use it any time you walk, jump, run, sprint, or even push up onto your toes.
While this tendon is structured to serve your body specific functions in terms of movement, that structure does weaken as you age. That increases its risk factors and susceptibility to injury, and this risk factor rises among those that see a sudden increase in their activity level. This can be people who end a sedentary work week to play hard physically on the weekend, but it can also be regular athletes who do suddenly increase the length or velocity of their workout sessions.
What Are The Symptoms Of Achilles Tendonitis?
 Knowing the specific symptoms of this injury is essential to identifying it and discerning it from other conditions. You also need to know them in order to know you have something more serious than normal aches and pains. However, the initial symptom you usually first notice with this injury is in fact a mild ache. It will either be above your heel or in the back of your lower leg. Occurrence of this shortly after playing a sport of going running is another indicator. Pain might be more than mild if you went through a long period of sprinting, running, or climbing stairs.
Knowing the specific symptoms of this injury is essential to identifying it and discerning it from other conditions. You also need to know them in order to know you have something more serious than normal aches and pains. However, the initial symptom you usually first notice with this injury is in fact a mild ache. It will either be above your heel or in the back of your lower leg. Occurrence of this shortly after playing a sport of going running is another indicator. Pain might be more than mild if you went through a long period of sprinting, running, or climbing stairs.
Pain is not the only symptom, as stiffness and tenderness might also present themselves. These might not show up until the morning after the triggering activity or event. These two symptoms often wane with mild activity throughout the day however.
If mild activity and attempts at self-care do not seem successful, and the pain seems persistent, contact your physician about your next steps. If, however, the pain is serious and you are actually disabled by the injury, get to a doctor or urgent care facility promptly. You possibly have torn or ruptured your tendon.
Age is not the only risk factor for risk of this injury. According to analysis of documented cases, Achilles tendonitis happens far more often to men than to women. Across both genders, physical problems exist that can put extra or unnecessary strain on these tendons. These problems include but are not limited to obesity, tight calf muscles, and naturally flat foot arches. If you suffer from any of these conditions, be sure to get a proper pair of shoes on your feet to support your bodyweight. Check out my overweight men’s and women’s shoe reviews.
Exercise choices have tremendous impact on the risk of symptoms developing, given the high correlation between athletic activity and Achilles tendonitis. Running in shoes that are worn out increases the chances of this injury, as does running up and down hilly or mountainous geography. Aches or pains in these tendons also happen more in colder climates and seasons than they do in warmer weather and times of year.
Physical conditions not directly related to exercise also increase risks of developing injury to the Achilles tendons. If you have high blood pressure or psoriasis, you are at increased risk. Also, specific kinds of antibiotics known as fluoroquinolones seem to have correlation with increased frequency of this injury, so be on the lookout for symptoms if you are prescribed such antibiotics. Do note, though, that not all antibiotics increase your risk factors.
How Is Achilles Tendonitis Specifically Diagnosed?
While the symptoms of this condition are specific enough that you can probably guess you have it on your own, a whole range of other issues can cause the same or similar symptoms, so it is best to have a medical professional make the official call. Light and mild cases might just mean a phone call to your physician, but moderate to severe cases usually dictate going in for an appointment.
Depending on your symptoms, your primary care physician might give you a reference to a specialist who has more concentrated experience, education, and training regarding matters like this. Sport medicine doctors are common specialists that step in here, but you might also be assigned to a physiatrist who specializes in rehabilitative or physical medicine. Actual tears and ruptures can mean being referred to orthopedic surgeons.
In order to streamline your appointments, it is useful to write down a list of questions you are likely to get asked. Doing this in advance means you do not have to struggle to think of answers while there or forget anything important. Questions you can expect to face include but are not limited to the following nine queries doctors and nurses might ask you:
- Was the onset of pain gradual or did it happen suddenly?
- What are you doing to manage or relieve your pain?
- Do symptoms get worse after particular activities or at different times of day?
- Did you recently change your workout pattern or start up a new activity?
- What kind of foot-ware do you wear during sports?
- Can you describe your typical workout routine?
- Can you list your regular supplements and medications?
- Does getting physical rest diminish the level of pain you feel?
- Where does it specifically hurt on your body?
When you undergo your physical examination, your physician is going to press gently on spots of the suspected or affected area of your leg. Your doctor does this, not to torture you as many patients fear, but instead to assess the specific location where the pain is present, as well as levels of tenderness and swelling. Other things your doctor is looking for include the range of motion, flexibility, reflexes, and alignment of your ankle and foot.
Additional tests using modern medical technology are often useful after the physical examination in determining the extent of severity of your tendonitis. An MRI or magnetic resonance imaging uses a combination of a powerful magnet and radio waves to give your doctor incredibly detailed imagery of your affected tendon.
X-rays are perhaps the oldest of the used technologies, but are very reliable in what they do. Soft tissue analysis isn’t possible, and tendons fall into that category. However, X-rays can be used to rule out different situations other than Achilles tendonitis that might trigger the same or related symptoms.
You might know of ultrasounds mostly from expecting mothers getting to know the gender of their babies, but they are also useful in creating live-time pictures of tendons in motion. Sound waves make visualization of the soft tissue possible, and color-Doppler ultrasounds can even analyze the circulation and flow of blood in and around your tendon.
How Do You Cure Achilles Tendonitis?
The overwhelming majority of cases of this injury are rather simple to take care of. You can care for yourself at home with supervision and guidelines from your physician. Caring for this ailment is essential, because tendonitis in the Achilles tendon can weaken it, which means it is at higher risk of an actual rupture or tear. In those serious cases, you are probably looking at surgery necessary for repair.
Self-care treatment should usually start with pain management. Over the counter pain relievers are a first step. Naproxen (found in Aleve and others) and ibuprofen (found in Motrin IB, Advil, and others) are good places to start. If none of these work, you might get a prescription medication that focuses on relieving pain and reducing your inflammation.
Orthotic devices like shoe wedges or inserts which elevate the heel are commonly used in cases of this injury or condition. They reduce the stress put on the tendon by providing a cushion that cuts down on the amount of work the tendons have to do.
Specific exercises are often chosen and trained by physical therapists on a case by case basis. These usually focus on strengthening and stretching both the tendons and their supporting tissues. Eccentric strengthening is noted for its effectiveness in healing repetitive Achilles tendonitis, and it involves raising a weight and then letting it down slowly.
Surgery is recommended in cases of severe pain and disability, confirmed tears or ruptures, and cases where multiple consecutive months of the aforementioned treatments fail to work.
Caring for yourself when recovering from this injury is condensed into the popular acronym R.I.C.E.:
- R stands for rest, which means skipping your workouts for a few days, or just switching to things that don’t stress or even use your Achilles tendon. This is a great excuse to spend some time in the swimming pool, if you have access to one. Crutches and walking boots might be needed during this phase if your situation is bad enough.
- I stands for ice, so anytime you do exercise or feel the pain setting in, put an ice pack on your afflicted tendon (hopefully it’s only one of them) for a quarter of an hour. That should reduce both your swelling and pain.
- C stands for compression, so use compressing elastic bandages or sports wraps to reduce both the ability of the tendon to move and also its swelling.
- E stands for elevation, so when you can, raise the affected leg above the height of your heart. This cuts down on swelling, and it is a great excuse to put on Netflix and literally put your feet up. If you are able to sleep with your foot elevated, this is extremely helpful.
How Do You Prevent This Injury From Happening Or Recurring?
Complete and total prevention of this injury is likely impossible. Having said that, there are five steps you can take to manage your risk and reduce the chances of occurrence from happening in the future:
- Stretch every single day. This habit is especially effective if you have had prior issues with your Achilles tendons. The three most-effective times to stretch include the early morning, and before and after your exercise sessions. Make sure to stretch both your Achilles tendons and calf muscles.
- Pick your shoes wisely. Worn-out shoes need replacing in all circumstances. New shoes should feature plentiful cushioning for your heels as well as solid arch support for your feet. Also consider adding heel and arch supports to otherwise good shoes that might be lacking in them.
- Build up your calves. Do specific exercises focused on making your calf muscles stronger so they can better support your Achilles tendons.
- Be easy on yourself. Don’t go running up hills when you can avoid it. If you must take part in something strenuous, workout at a slow pace at start so you can warm your body up. If any particular activity triggers pain, stop immediately and take a break.
- Increase your intensity and duration in a gradual manner. If you are new to working out or just getting back into it, start small and build. Likewise, if you’re already used to working out, don’t suddenly double your duration or intensity.
- Do cross-training. Jumping, running, tennis, and basketball are all high-impact activities on your legs. When you can switch things up with low-impact alternatives, such as swimming and cycling. It’s better for your body, and can take the repetitive boredom out of your overall fitness regimen.
Achilles tendonitis can happen to anyone at any age. However, it seems to happen most to men, those in middle age, and those that participate in high-impact sports, particularly when there is a sudden jump in their activity level. Use all that you have learned here to watch out for tendonitis in your own Achilles tendons, as well as how to treat it and reduce your future risks of occurrence.

Great info. I just bought a pair of casual/dress boots. And I have a pair of Superfeet Trailblazers insoles in them. I might have worn them too long today without breaking them in. But by the end of a long day shopping and running all over town, I noticed that my Achilles really hurt with every step. I’m hoping that this will change as my feet get used to wearing the boots and they get broken in. Cheers! -Kristian
Hi Kristian,
I hope so, too. If not, then you can always try Tread Labs insoles, instead.
Let me know how it works out for you.
Sincerely,
Brian